Blog
Hear from our experts
Our expert employees are not only focused on healing injured workers, but also contributing to the industries we serve.

10 Work Comp Did-You-Knows
Physical and occupational therapy are excellent approaches to addressing musculoskeletal problems after a workplace injury. Workers’ compensation cases can be difficult to navigate for employers, workers, and therapy providers. In honor of Bardavon’s 10th year, …
Read More
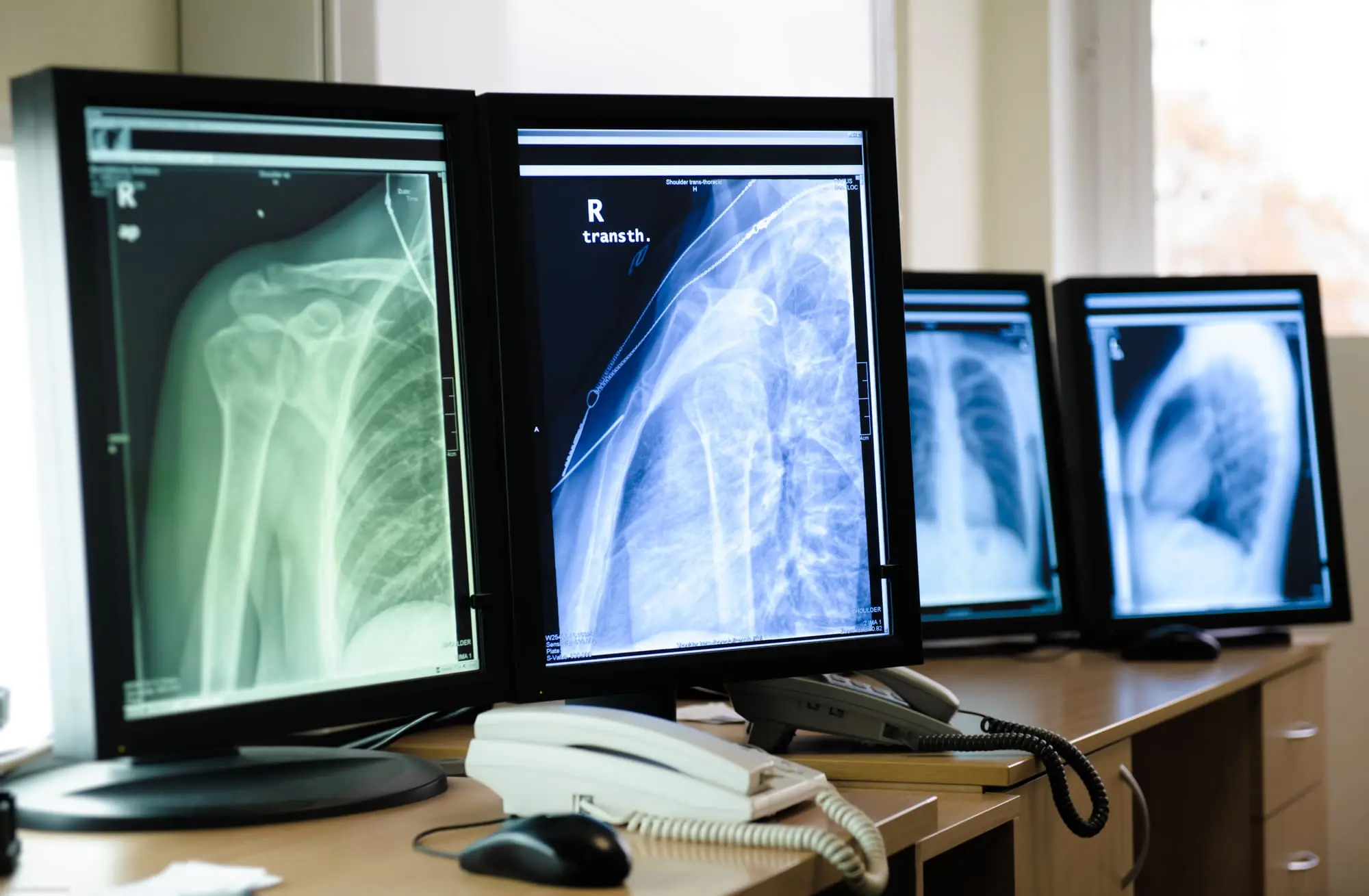
Navigating Imaging Referrals in Physical Therapy: From Direct Access Empowerment to Responsible Imaging Referrals
Synopsis The American Physical Therapy Association (APTA) and its regional chapters have successfully advanced the cause of direct access for physical therapists, positioning them as primary care specialists for musculoskeletal health. This achievement has led …
Read More

Cameras and Computer Vision: Accurately Capturing Human Movement with Injury Prevention Tech
New technology has entered the world of prevention to assist and identify movement patterns and tasks that can be modified to help decrease musculoskeletal injuries and protect workers. Cameras have become one of the most …
Read More

Injury Prevention Case Study: Insurance Carriers and Brokers
Reduce Musculoskeletal Claims Volume Using Wearable Technology and Data Analysis Accounting for nearly half a million injuries per year, MSDs represent one-third of all workers’ compensation costs, resulting in direct costs of more than $20 …
Read More

